Drug treatment of children with respiratory tract infections
Purpose
The aim of this report is to identify all systematic reviews with low or moderate risk of bias on drug treatments for children with respiratory tract infections, to systematically and transparently describe the extent of research in the field, and to identify gaps in the research base.
What does this evidence map add?
The result from this scoping review demonstrates that a large number of treatments given to children have not been evaluated in any systematic review of low or moderate risk of bias. This report is a summary of existing systematic reviews in the field and should not be used as treatment guidelines.
Background
Respiratory tract infections are the most common infections seen in school-aged children, with 7 to 10 infections a year being considered normal. Most respiratory tract infections are caused by viruses and heal without any treatment. However, antibiotic treatments are prescribed to children between the ages of one and seven with respiratory tract infections more often than to older children and adults. Fever and other symptoms associated with respiratory tract infections are also more commonly treated with medication in children aged 1–7. This report was initiated by the Medical Products Agency after consulting professional organizations in this field.
Method
A mapping of systematic reviews to domains considered important by pediatricians in their daily clinical practices was undertaken (see table below). After searching several electronic databases for systematic reviews relevant to the identified domains, two reviewers independently screened the abstracts for relevance. Identified full text reviews were then assessed independently by two reviewers for relevance and thereafter methodological quality using AMSTAR. Differences were resolved by consensus. Systematic reviews judged to have low or moderate risk of bias were then used to assess the current body of evidence, including identifying those domains where insufficient evidence is available.
Main results
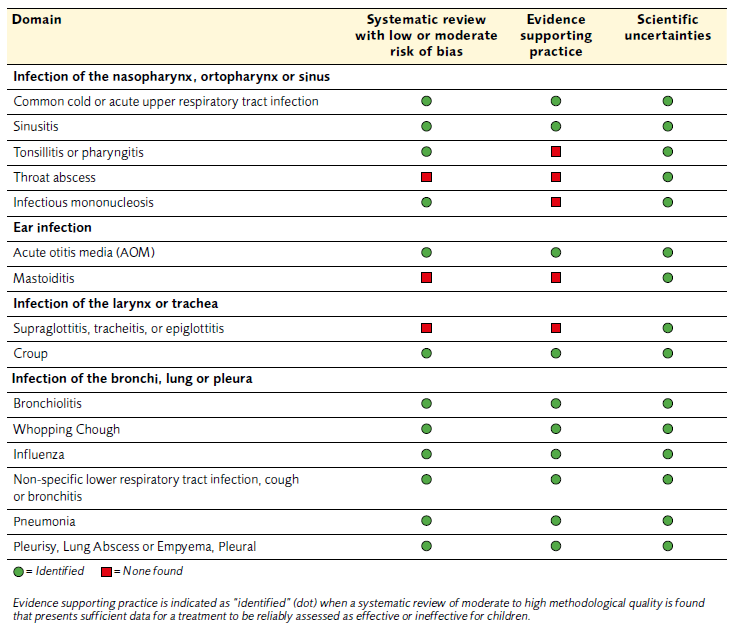
Out of the 165 systematic reviews meeting the inclusion criteria, 72 were judged to have a low or moderate risk of bias. Within the body of evidence we found evidence to support practice in some of the identified pediatric healthcare domains. However, no systematic reviews with low or moderate risk of bias were identified assessing the treatment of throat abscesses, mastoiditis, epiglottitis or tracheitis.
Table 1 Domains, evidence supporting practice and scientific uncertainties obtained from systematic reviews of high or moderate quality.
Project group
Experts
- Sten Erik Bergström, MD, PhD, Consultant paediatrician
- Ann Hermansson, MD, Associate professor, Consultant ENT surgeon
- Inge Axelsson, MD, Professor, Consultant paediatrician
- Ingemar Tessin, MD, PhD, Consultant in pediatrics and neonatology
SBU
- Christel Hellberg (Project Manager, Information Specialist)
- Frida Mowafi (Assistant Project Manager, Information Specialist)
- Anna Attergren Granath (Project Administrator)

 Swedish Agency for Health Technology Assessment and Assessment of Social Services
Swedish Agency for Health Technology Assessment and Assessment of Social Services
 Share on Facebook
Share on Facebook
 Share on LinkedIn
Share on LinkedIn
 Share via Email
Share via Email