This publication was published more than 5 years ago. The state of knowledge may have changed.
Value-Based Health Care – a mapping of the literature
A mapping of the literature
This systematic mapping suggests that research on Value-Based Health Care is limited, especially on the framework in its entirety. Existing research often has shortcomings and shows great variation in how Value-Based Health Care has been applied.
Aim
Health care faces economic, demographic, and medical challenges. How health care is managed and organised can provide ways to address these challenges. On behalf of the Swedish government, SBU has performed a systematic mapping of published research on the Value-Based Health Care framework. The resulting report provides an overview of the research available today. The results show how the framework has been evaluated in published scientific articles, in which contexts, and with which research methods. We have not evaluated the evidence, nor assessed if the conclusions of the included studies are transferable to other health care organisations within Sweden or internationally.
Background
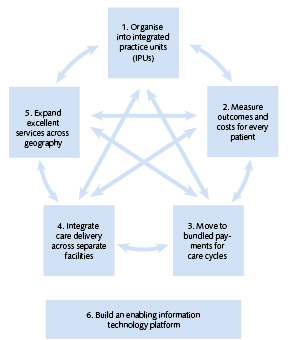
Value-based Health Care offers a framework to which various management and organisational methods, interventions, and approaches can be linked in order to achieve the best possible value, defined as health outcomes for patients in relation to the costs incurred to achieve those results. It requires a shift in focus away from volume towards (competition on) the quality and costs of produced care. The framework for Value-Based Health Care involves six interconnected strategies, referred to as “the value agenda” (Figure 1).
Various interpretations of the framework have emerged since Value-Based Health Care was first introduced by Porter and Teisberg in 2004. The framework has also developed since then, and it has been applied in different ways.
Method
A systematic literature search was performed in six databases covering the period January 2014 to December 2017. The search was supplemented with a citation search based on two central articles written by Porter and co-authors. Only studies that evaluated Value-Based Health Care were included. The subject of the evaluation presented in the study had to either be termed Value-Based Health Care or Value-Based Care. Additional evaluation studies were included, provided that the authors of the study described it as Value-Based Health Care according to Porter and co-authors’ framework. The studies also had to contain an analysis of collected data and the intervention or measure being studied had to have been carried out within a health care organisation or system. The studies were analysed thematically. Additional analyses were carried out to identify the program theories, i.e. the basic assumptions and theories of how Value-Based Health Care was intended to work.
Results and discussion
In total, 36 articles were found to be eligible for inclusion. The number of published scientific articles has increased in recent years; 16 of the 36 articles were published in 2017. Most articles came from Western countries where American articles dominated (22 out of 36). Of the six Swedish articles, five studies looked at Sahlgrenska University Hospital and its implementation of Value-Based Health Care. Many (14 of 36) of the included articles were simple case reports whose analyses and results must be considered preliminary. The articles had different perspectives; a majority took the health care provider’s viewpoint (for example, a clinic or a hospital) and only a few included patient perspectives, albeit limited.
Few studies examined the full framework of Value-Based Health Care, i.e. all six strategies of the value agenda. The research largely focused on individual components, primarily related to outcomes and costs. This means that we only have a limited amount of evidence to support any general conclusion about the effects and results of Value-Based Health Care. Further, it is unclear whether studies on individual components can be used to support general conclusions on the impact of Value-Based Health Care on efficiency or efficacy, since the individual components are not unique for Value-Based Health Care, but also exist alone or as components of other organisational models and frameworks.
The included studies had several limitations. The study design was often inadequately described. In several studies it was unclear when and how the data were selected, collected, or analysed. Furthermore, the studies were relatively heterogeneous with, for example, different medical conditions or settings (e.g. cancer, hip joint surgery, myocardial infarction or children with complex conditions), outcome measurements, and cost variables.
The results of the articles indicate that the components of Value-Based Health Care may have a positive impact on health outcomes and reduced care time. However, it is not possible to draw generalisable conclusions regarding specific effects of Value-Based Health Care based on these studies. The results do indicate that the development of meaningful outcomes and other components of Value-Based Health Care may benefit from actively involving business representatives, patients, professionals, and experts to better understand what works for whom and under what conditions.
Future research
Future research should focus on systematic, critical, and theory-driven investigations of interventions based on a systems view of the context and process in which the Value-Based Health Care framework is applied. Important aspects to consider are patients’ experiences of Value-Based Health Care, working environment conditions for health care professionals, and transitions between health care units within and between hospital organisations. The methodology of research also needs to be developed to handle multidisciplinary research questions and the type of ambiguous results that emerge when studying complex social interventions and innovations. Multidisciplinary research groups are probably situated in a favourable position to evaluate Value-Based Health Care from the different perspectives of the involved stakeholders.
Reference
Porter M, Lee T. The strategy that will fix health care. Harvard Business Review 2013;91.
Full report in Swedish
The full report in Swedish "Värdebaserad vård – kartläggning av kunskapsläget"

Project group
Experts
- Lotta Dellve (Professor)
- Andreas Hellström (Senior Lecturer, PhD)
- Charlotta Levay (Associate Professor)
- Carl Savage (PhD)
SBU
- Jenny Odeberg (Project Manager)
- Per Lytsy (Assistant Project Manager)
- Anna Ringborg (Health Economist)
- Caroline Jungner (Project Administrator)
- Maja Kärrman Fredriksson (Information Specialist)
 Swedish Agency for Health Technology Assessment and Assessment of Social Services
Swedish Agency for Health Technology Assessment and Assessment of Social Services



